How Minimally Invasive Surgery Has Changed the Healthcare Industry
Aug. 1 2019, surgicaladmin
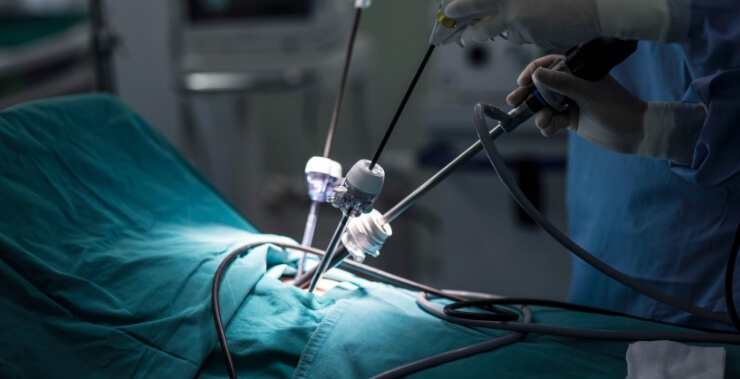
Minimally invasive surgery is contrasted from open surgery because of its nature: instead of opening the body and cutting through large areas of tissue to operate, a surgeon will make small surgical incisions to gain access to the body and its organs, thereby allowing them to operate faster with much less injury and damage to the patient. Additionally, this reduced stress on the body also translates to a shorter hospital stay with fewer complications. In fact, many minimally invasive procedures are considered outpatient surgeries in which the patient does not need to stay overnight in a medical facility.
As such, minimally invasive surgery has become a standard surgical technique in many routine operations that include:
● Adrenalectomy to remove one or both adrenal glands
● Appendectomy to remove the appendix
● Cancer surgery to destroy a tumor
● Cholecystectomy to remove the gallbladder
● Colectomy to remove parts of a diseased large bowel
● Endovascular surgery to treat or repair aneurysms
● Hiatal hernia repair to relieve gastroesophageal reflux disease
● Splenectomy to remove the spleen
As well as the following treatment areas:
● Colon and rectal surgery
● Ear, nose and throat surgery
● Gastroenterology surgery
● General surgery
● Gynecology surgery
● Heart surgery
● Kidney surgery
● Living donor kidney transplants
● Neurosurgery
● Orthopedic surgery
● Thoracic surgery
● Urologic surgery
For the most part, though there are many forms of minimally invasive surgery, most can be grouped into three general areas that include laparoscopy/endoscopy in which surgery is accomplished by a human with small tubes and tiny cameras and surgical instruments passed through one or more small incisions in the body or digestive tract, and robotic surgery in which surgical robots controlled by a surgeon with a magnified, 3D view of the surgical site do the operating. All of these lead to the advantages of minimally invasive surgery we touched on earlier like less pain, faster recovery and better results, as well as an additional one of reduced healthcare costs that we’ll go over in more detail later on.
To simplify things, let’s break these down into two broad categories—better outcomes and lower costs—that can better explain our topic today: how minimally invasive surgery has changed the healthcare industry.
Better Outcomes
It is easy to see how minimally invasive surgery leads to better outcomes with fewer postoperative complications. After all, surgery that does not involve making large incisions and instead relies on small ones that can be used for the insertion of thin tubes, cameras, fiber optic lights, and small surgical tools is already safer because of that very fact.
Apart from this, minimally invasive surgery is also associated with less pain and discomfort. In fact, studies have found that patients recovering from minimally invasive surgery report less pain and need smaller doses of pain relievers than patients who have undergone open surgery. Along similar lines, smaller incisions lead to less blood loss and faster recovery times, allowing patients to go back to their normal routines much sooner than if conventional surgery was used. Because minimally invasive surgery requires smaller incisions with fewer stitches, smaller and less noticeable scars are another advantage gained from it.
With the use of a camera that allows for better visualization by opening up the entire operative field, minimally invasive surgery also comes with a higher accuracy rate compared to open surgery. This is even truer when considering robotic surgery, which also leads to higher precision, flexibility, and control with the use of mechanical elements paired with feedback-controlled motions. In use, this creates actions that are much smoother than anything achieved with a human hand, especially because adjustments to scale can be made to make every move much more precise (e.g. a three-to-one scale would move a robot’s arm one inch for every three inches that the hand of a surgeon or surgical technician moves).
Lower Costs
Along with better outcomes and less collateral damage associated with minimally invasive surgery come lower overall costs. In fact, not only did a nationwide analysis of surgical outcomes conducted by Johns Hopkins conclude that the use of minimally invasive surgery for certain common procedures can dramatically reduce post-operative complications, but also eliminate hundreds of millions of dollars from the nation’s healthcare bill. More specifically, it was concluded that American hospitals could collectively prevent thousands of post-surgical complications and save between $280 million and $340 million every year by using opting for minimally invasive surgeries instead of open surgery for routine operations of the appendix, colon and lungs.
Breaking down the numbers, it was discovered that 3,578 complications could be averted, hospital stays could be reduced by 144, 863 days, and $288 million a year could be saved if all hospitals in the U.S. increased the number of minimally invasive procedures by 50%. If, on the other hand, hospitals performing the fewest minimally invasive operations increased their levels to match those of their higher-performing counterparts, a collective 4,306 fewer complications could be averted, there would be 169,819 fewer hospital days, and $337 million a year could be saved.
Final Thoughts
Minimally invasive surgery is surging in popularity, as exemplified by a new market intelligence report by BIS Research that found that the global market for minimally invasive surgical systems is estimated to grow over $40.52 billion by 2025 at a CAGR of 10.9%. As we saw today, this increased demand for minimally invasive surgery is spurred by the many advantages it offers over traditional open surgery that include less pain, smaller and fewer scars, shorter hospital stays and recovery periods, reduced costs, and overall better outcomes. This demand has also given rise to many organizations like Surgical Solutions that offer minimally invasive surgical support for these types of procedures, allowing even more facilities to leverage this surgical technique for their own patients.
surgicaladmin
Administrator



